Scarring Alopecia: Background, Pathophysiology, Epidemiology
Maybe your like
A systematic approach to the evaluation of alopecia enables more effective management. The usual first step is to establish whether the alopecia is scarring (cicatricial) or nonscarring, as follows:
- Nonscarring alopecias - Follicular ostia tend to be preserved; no clinically visible inflammation is usually noted, though histologic inflammation may be present; the most common nonscarring alopecias are alopecia areata and telogen effluvium
- Scarring alopecias [1] - Loss or atrophy of follicular ostia occurs; clinical inflammation is frequently (but not always) present, and histologic inflammation may be present; ultimately, histologic confirmation is the best method for confirming the presence of a fibrosing/scarring process with loss of hair follicles
Many alopecia types are biphasic. For example, androgenetic alopecia eventually results in loss of ostia and thus may resemble a scarring alopecia. This article focuses on the alopecia types that are believed to be due to an inflammatory response with rapid secondary scarring if not controlled.
Once it has been established that the patient has scarring alopecia, it is important to identify the specific type and apply the appropriate clinical-based terminology so as to facilitate confirmation of the diagnosis, initiation of treatment, and determination of the prognosis. Several manuscripts have examined and attempted to clarify the literature findings, [2, 3, 4] as summarized below.
It is essential to note that examination, by itself, cannot be the final diagnostic step; the alopecia literature is filled with examples of misdiagnosis and diagnostic mimics. [5, 6, 7, 8] For instance, some patients present with nonscarring, noninflammatory alopecia that is later found to be scarring and inflammatory. [9] Even within the scarring alopecia presentation, there has been debate regarding the relative roles of immune alteration and purely external factors as causes of the alopecia. Much of the diagnostic confusion arises from the similarities of clinical presentation, again emphasizing the importance of not basing diagnosis solely on clinical examination findings. [10]
Diagnoses with predominance of lymphocytes
Lichen planopilaris
The diagnosis of lichen planopilaris (LPP) is confirmed by a combination of clinical and histologic features. The following potential clinical variants are recognized [11] :
- Frontal fibrosing alopecia (FFA; see the image below) - This variant has histologic features similar to those of LPP; it has been associated with the postmenopausal state (ie, postmenopausal frontal fibrosing alopecia), though not all patients with this diagnosis are postmenopausal
- Fibrosing alopecia in pattern distribution (FAPD) - This variant also has histologic features similar to those of LPP, as well as some histologic and clinical overlap with androgenetic alopecia; it may also reflect an overlap of LPP with androgenetic alopecia.
- Graham-Little syndrome - This is another possible overlapping condition, with features of LPP and other alopecia types
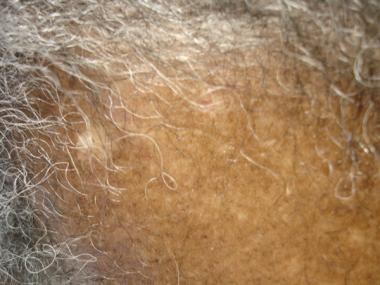 End-stage scarring alopecia (ESSA) with prior history of itching and burning, along with receding hairline. Started as lichen planopilaris (LPP) variant frontal fibrosing alopecia (FFA). Image from Rashid M Rashid, MD, PhD, Morzak Research Collaborative. View Media Gallery
End-stage scarring alopecia (ESSA) with prior history of itching and burning, along with receding hairline. Started as lichen planopilaris (LPP) variant frontal fibrosing alopecia (FFA). Image from Rashid M Rashid, MD, PhD, Morzak Research Collaborative. View Media Gallery Central centrifugal cicatricial alopecia
Central centrifugal cicatricial alopecia (CCCA) is a diagnostic category adopted by the American Hair Research Society (AHRS) to encompass terms such as hot comb alopecia, follicular degeneration syndrome, pseudopelade in African Americans, and central elliptical pseudopelade in whites. [11] Despite the many attempts to clarify and unify the terminology of central CCCA patterns of scarring alopecia, CCCA has not been clearly established as a diagnostic entity in and of itself.
Pseudopelade
Pseudopelade is a term used to describe a clinically noninflammatory patchy alopecia. The most common condition producing this appearance is LPP. The term idiopathic pseudopelade refers to a distinct fibrosing alopecia characterized by a thin dermis, with dense eosinophilic dermal collagen and thick recoiled elastic fibers. The fibrous tracts are broad and may contain granulomas, but the surrounding elastic sheath is preserved.
Traction alopecia
As the name implies, traction alopecia is alopecia secondary to physical traction. Variant presentations exist with terminology that is optional for the purposes of differentiation. This terminology includes alopecia linearis frontalis (ALF), more commonly known as marginal alopecia, and chignon alopecia, which is used when a tight hair bun causes the traction changes.
Secondary systemic scarring alopecia
Secondary systemic scarring alopecia is a term used when the alopecia is a feature of a systemic disease (eg, scleroderma or discoid lupus erythematosus [DLE]). DLE is a frequent cause of alopecia. In the classic lupus classification scheme, DLE is one of the chronic cutaneous lupus types (along with tumid lupus and lupus panniculitis).
Trichotillomania
Trichotillomania is a nonscarring psychiatric alopecia that can have a scarring clinical presentation. Trichotillosis is an alternative term that some physicians believe is more acceptable to patients. [12]
Chemotherapy alopecia
Chemotherapy alopecia is often thought of as a nonscarring alopecia; however, reports of permanent alopecia suggest that hair stem cells can be permanently destroyed. (See the image below.)
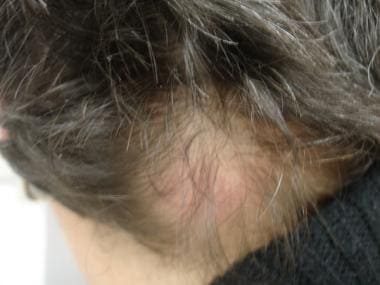 Alopecia due to primary cutaneous follicular center cell lymphoma. Image from Rashid M Rashid, MD, PhD, Morzak Research Collaborative. View Media Gallery
Alopecia due to primary cutaneous follicular center cell lymphoma. Image from Rashid M Rashid, MD, PhD, Morzak Research Collaborative. View Media Gallery Alopecia mucinosa
Follicular mucinosis can exist by itself or can be a manifestation of mycosis fungoides.
Keratosis pilaris atrophicans
Keratosis pilaris atrophicans involves a spectrum of conditions that resemble keratosis pilaris but result in hair loss.
Diagnoses with predominance of neutrophils
Folliculitis decalvans
Folliculitis decalvans presents with recurrent crops of follicular pustules that result in permanent epilation. Staphylococci are often cultured from pustules, but this condition does not respond to the standard antibiotic regimens. The best results are obtained with long-term use of topical corticosteroids together with an oral tetracycline.
Perifolliculitis capitis abscedens et suffodiens
Other terms used for perifolliculitis capitis abscedens et suffodiens include dissecting cellulitis of the scalp and Hoffman disease. This condition resembles hidradenitis suppurativa, and the two often occur together.
Tufted hair folliculitis
Tufted hair folliculitis often contains Staphylococcus aureus, but it is unclear whether a preexisting abnormality predisposes to staphylococcal infection. Clinically, five to 20 hairs emerge from a common dilated follicular orifice (see the image below), producing a clinical resemblance to doll hair. This is often seen as a reactive pattern present in multiple types of scarring alopecia and even as a reaction to medications. [13]
 View Media Gallery
View Media Gallery Diagnoses with predominance of mixed cell types
Acne keloidalis
Others terms used for this condition include acne keloidalis nuchae, dermatitis papillaris capillitii, sycosis nuchae, and folliculitis keloidalis. Patients present with pustules, alopecia, and hypertrophic scarring on the posterior neck. Many plasma cells are typically present in the infiltrate.
Acne necrotica
Acne necrotica, sometimes referred to as folliculitis necrotica, is a rare condition that exists in the following two variants:
- Acne necrotica varioliformis, which is a distinctive necrotizing disorder of the hair follicle that heals with varioliform scars
- Acne necrotica miliaris, which is a nonscarring folliculitis
Erosive pustular dermatosis of the scalp
This condition often follows surgery or other trauma. It presents with an expanding patch of crusts and pustules. [14] It has been reported to respond to potent topical corticosteroids, tacrolimus, and light therapy.
Diagnoses less well characterized
Pressure alopecia
Pressure alopecia is due to constant pressure on the region. Although it is often described as a nonscarring reversible alopecia, it has been reported to result in permanent scarring. Pressure alopecia may be more accurately termed externally traumatic alopecia or iatrogenic alopecia. [15] As in chemotherapy alopecia, the rapidly growing hair follicle and hair cell source (bulge and associated regions) may be especially susceptible to antimetabolic insult, such as lack of blood flow.
Lipedematous alopecia
Lipedematous alopecia is a rare condition with unknown scarring potential. It is also referred to as lipedematous scalp.
Senescent alopecia
Senescent alopecia, also known as senile alopecia, is a diffuse thinning that is due to decreased terminal hairs but without increased miniaturization. [16] It is thought to affect people aged 40-50 years or older with no family history or evidence of pattern balding. Senescent alopecia is not a primary diagnosis in all clinics, and there has been debate as to whether it is an actual diagnosis or a form of late-onset androgenetic alopecia. [17]
Keratosis follicularis atrophicans
Possible variants include keratosis pilaris decalvans, an X-linked and sporadic condition, and keratosis follicularis spinulosa decalvans, which is autosomal dominant.
Tag » What Does Scarring Alopecia Look Like
-
Scarring Alopecia Symptoms, Causes, Treatments, And More
-
Scarring Alopecia - Symptoms, Causes, Treatment & Prevention
-
Cicatricial (Scarring) Alopecia - Treatment, Causes, Symptoms
-
SCARRING/CICATRICIAL ALOPECIA | Prescription Haircare
-
What You Should Know About Scarring Alopecia - Vegamour
-
Overcoming Scarring Alopecia: Symptoms & Treatment Options
-
Lichen Planopilaris (Scarring Alopecia)
-
Scarring Hair Loss - Wikipedia
-
Scarring Alopecia: Symptoms, Causes & Treatment - Hims
-
Scarring Alopecia Specialist - Marc Avram, MD
-
Feature Characterization Of Scarring And Non-scarring Types ... - NCBI
-
Cicatricial Alopecia - National Organization For Rare Disorders
-
Scarring Alopecia: Types And Treatments - Health Guide